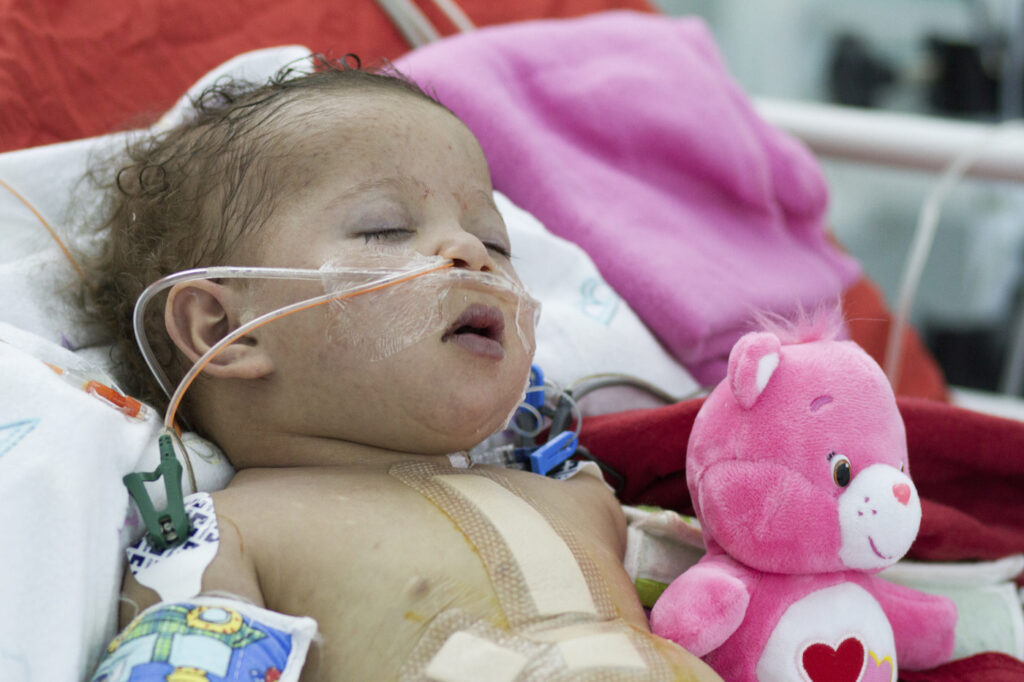
6pm in the ICU
Libya. Wednesday, 5:57 pm. ICU. We’ve dimmed most of the lights, so the patients can sleep more easily. Sleep is valuable medicine. Rouana’s mom sits beside her, gently cleaning tape scum off of her face with a damp piece of gauze, then feeding her a bottle. She talks in a soft voice, tipping her head …