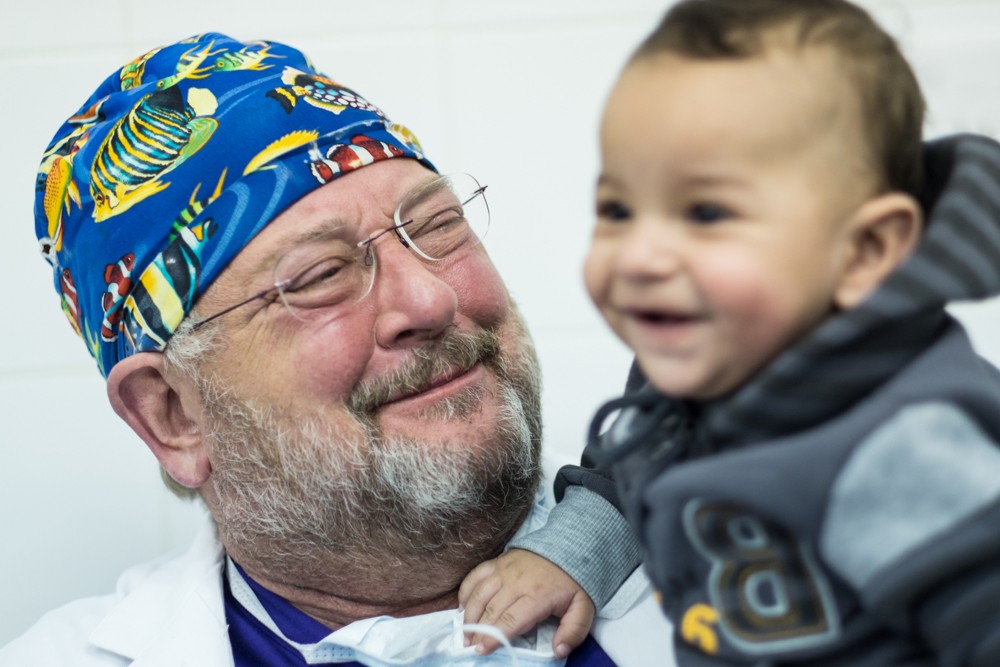
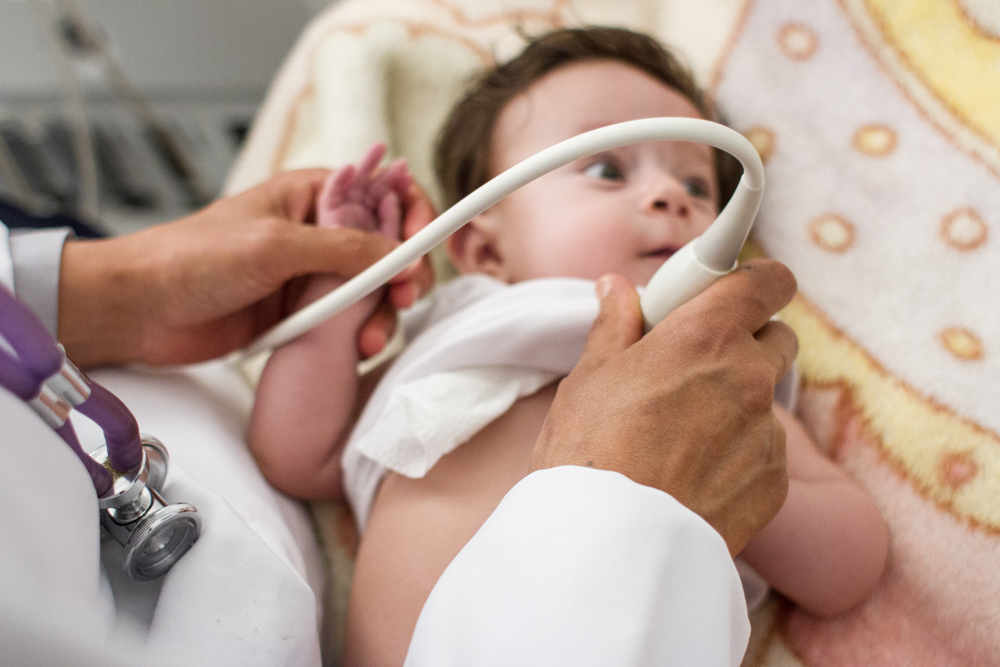
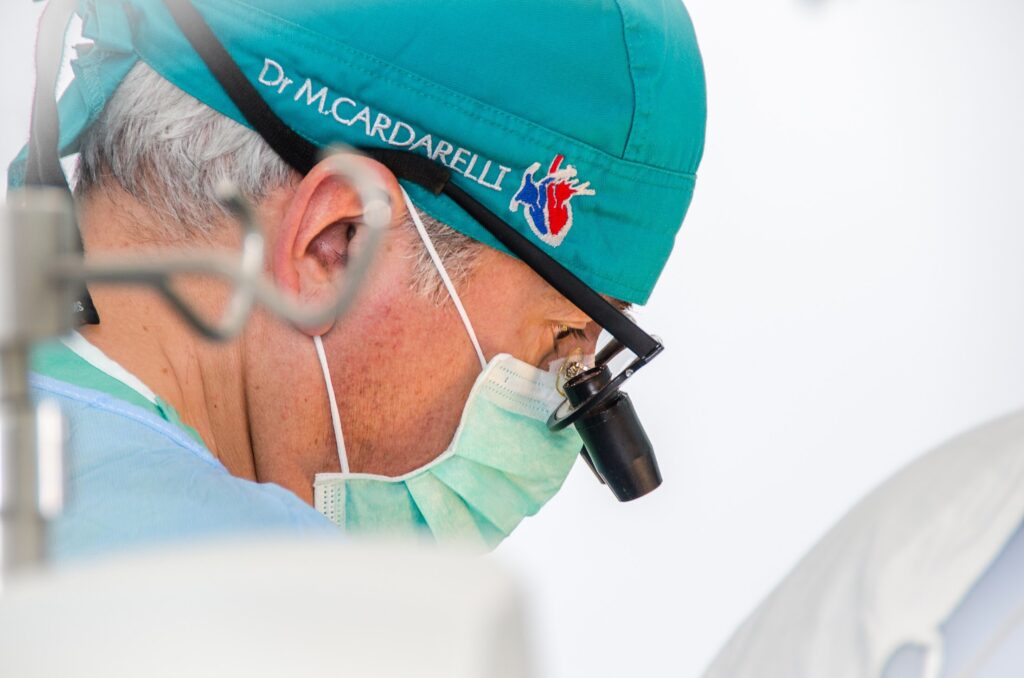
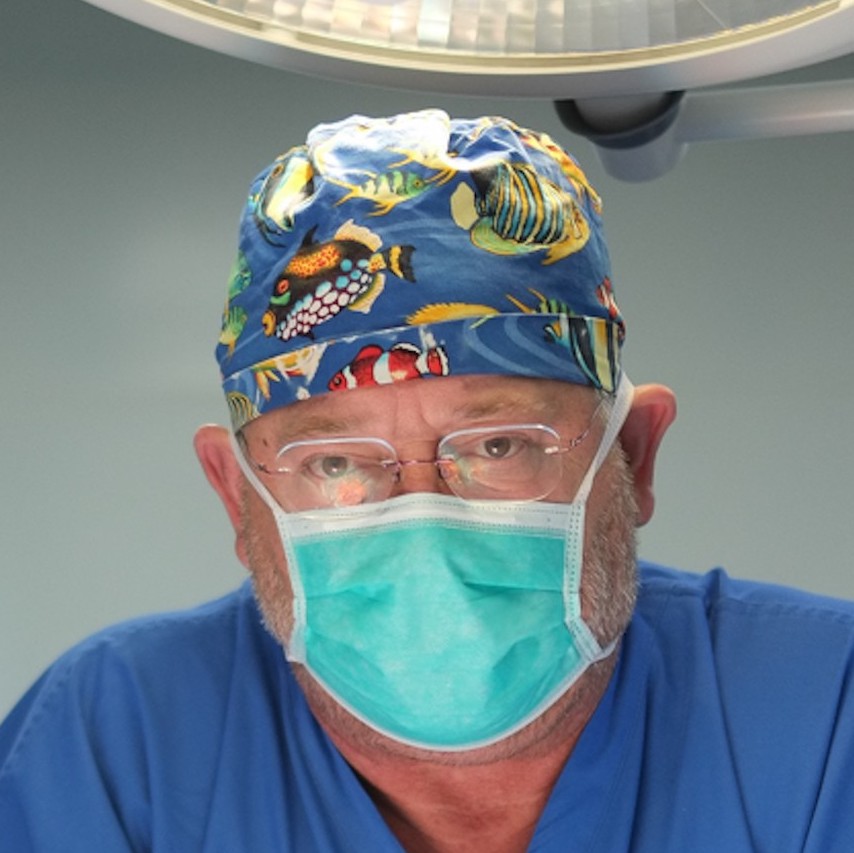
John Hopkins fellow Meghan Halub joins Dr. William Novick in Libya & Ukraine
Society of Thoracic Surgeons Global Outreach Fellowship Award Recipient Chooses NCA Meghan Halub, a second-year cardiothoracic surgery Fellow at Johns Hopkins Hospital joined NCA teams last fall in Benghazi, Libya and Kiev, Ukraine. Dr. Halub’s experience was recently published in Annals of Thoracic Surgery: